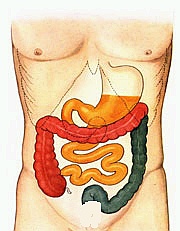
 The human digestive system is colonised by several hundred bacterial species or gut microflora. The large intestine is the most heavily colonised area of the human body and the stomach is the least colonised due to its acidic environment.
The human digestive system is colonised by several hundred bacterial species or gut microflora. The large intestine is the most heavily colonised area of the human body and the stomach is the least colonised due to its acidic environment.
Certain strains and amount of gut microflora are acquired at birth, but later on, the strains and amount varies in the individual. This depends on the individual age, the type of diet and history of insult to the digestive system.
The gut microflora are also called commensal bacteria, meaning they live within and benefit from humans without causing any harm. Commensal bacteria evolved together with humans, several species are now considered beneficial such as bifido-bacteria and lactobacilli, however, other are considered harmful such as clostridia and bacteroides due to toxin production and ability to promote certain types of cancer.
Numerous research showed that beneficial bacteria has the ability to influence the three line of defences in the gut; by repressing invading organism, improving the gut barrier function and increases the gut immunity. For these reasons, scientists and researchers are able to justify the importance of maintaining the appropriate species and amount of beneficial bacteria in our gut, which leads to the development of “probiotics”.
 Probiotics as defined by the World Health Organisation (WHO) is “Live micro-organism which, when administered in adequate amounts confer benefits on the host”.
Probiotics as defined by the World Health Organisation (WHO) is “Live micro-organism which, when administered in adequate amounts confer benefits on the host”.
Many different species of bacteria had been used as probiotics but the most common are bifido-bacteria and lactobaccili. Guidelines from the Food and Agriculture Organisation (FAO) and WHO was set in 2002 to ensure that foods claimed to have probiotic health effect were evaluated for the use of appropriate probiotic strain, safety for human consumption with appropriate health claim and labelling.
Probiotics are available in the market in the UAE and marketed as health and functional food. It is estimated that well over 10 million consumer in the Europe consume probiotics regularly (each day). The food vehicles for probiotics include live yoghurt, fermented dairy drinks, freeze dried supplements and fruit juices.
Probiotics had been used in studies carried out particularly in gastrointestinal infection, irritable bowel syndrome (IBS) and inflammatory bowel diseases (Chron’s Disease, Ulcerative Colitis). Gastrointestinal infections or gastroenteritis can cause severe diarrhoea and dehydration, leading to morbidity and mortality especially in underdeveloped countries.
 A review article on probiotics and gastrointestinal infections highlighted the usage of probiotics in the prevention and treatment of gastroenteritis. Several studies conducted in different countries, documented that there were less cases of acute diarrhoea in children supplemented with daily probiotics. In another study, small children with viral gastroenteritis treated with probiotics also had shorter duration of illness and recovered earlier. The findings were also supported by a recent (2008) compilation of data on scientific trials of probiotics concluding that probiotics appears to be affective in the prevention of gastroenteritis in children and reduces the duration on the illness.
A review article on probiotics and gastrointestinal infections highlighted the usage of probiotics in the prevention and treatment of gastroenteritis. Several studies conducted in different countries, documented that there were less cases of acute diarrhoea in children supplemented with daily probiotics. In another study, small children with viral gastroenteritis treated with probiotics also had shorter duration of illness and recovered earlier. The findings were also supported by a recent (2008) compilation of data on scientific trials of probiotics concluding that probiotics appears to be affective in the prevention of gastroenteritis in children and reduces the duration on the illness.
IBS is a chronic condition characterised by unspecific abdominal symptoms such as abdominal pain, indigestion, flatulence and nausea in the absence of any structural abnormality of the digestive system. It is difficult to pin point the exact cause of IBS although more recently it was associated with gut inflammation and altered composition of gut microflora. Usage of probiotics had been linked to improvements of symptoms in IBS. A study carried out on 77 patients with IBS, showed that patients given drinks supplement with 1×1010 live bifidobacteria for 8 weeks had overall improvements in symptoms. Furthermore, an analysis carried out on 23 clinical trials with over 1000 patients using probiotics as treatment of IBS showed there were overall improvements of symptoms especially with abdominal pain.
IBD includes Chron’s Disease (CD) and Ulcerative Colitis (UC). Unlike IBS, the disorder is characterised by chronic inflammation of the digestive system. The cause is unknown but it has been connected to altered gut microflora, with less beneficial bacteria and more harmful bacteria causing abnormal immune activity in the digestive system. Clinical trial carried out on patients with chronic UC, using highly concentrated 3 different strains of probiotics taken daily for 12 months, showed that relapse were fewer in the patients taking probiotic compared to those who did not. On the contrary, the benefits of probiotics could not be demonstrated in the treatment of CD. Studies carried out showed equivocal results and very few showed positive results.
In conclusion, probiotics consumption showed many benefits, however they have to be consumed regularly for the benefit to show. Once consumption ceases the effect will also cease. Currently there has been no documented side effect with consumption of probiotic other than mild feeling of bloatedness.
References:
1. Guidelines for the evaluation of probiotics in Food. Report of a joint FAO/WHO Working Group on Drafting Guidelines for the Evaluations of Probiotics in Food. London Ontario, Canada. April 30 and May1, 2002.
2. Booklet from Yakult. Probiotics in Health and Diseases. 2008.
3. Britton, R.A. and Versalovic, J. (2008). Probiotics and gastrointestinal infections. Interdisciplinary Perspective of Infectious Diseases. Volume 2008, Article ID 290796, 10 pages.
4. Gionchetti et al. (2003). Prophylaxis of pouchitis onset with probiotic therapy: a double-blind, placebo-controlled trial. Gastroenterology. 124:1202-1209.
5. McFarland, L.V. and Dublin, S.(2008). Meta-analysis of probiotics for the treatment of irritable bowel syndrome. World Journal of Gastroenterology. May7;14(17): 2650-2661.
Article Written by Sharliza Mohd. Saleh for Biomed Middle East

how can you saw that gut microflora will repress the invading microbes and how these gut microbes willsurvive under high alkaline and salt cnditions in the intestine. i wont agree that they wil repress the invading microbes. if the invading microbe is strong enoughwat the intestinal microflora will do. the are many microbes which will over cum the effect of probiotics. i want your jestification.